Prepared by Professor Alan Whiteside, OBE, Chair of Global Health Policy, BSIA, Waterloo, Canada & Professor Emeritus, University of KwaZulu-Natal – www.alan-whiteside.com
Introduction
This week there were just under 15 million Covid-19 cases globally. The USA accounts for the most, at around 3.9 million cases. South Africa is in fifth place, with Brazil second, India third, and Russia fourth. Peru, Mexico, Chile, the United Kingdom, and Iran make up the balance of the top ten. The global curve of new cases appears to be steepening.
In this week’s communique I am delighted to include a guest column by Katherine Marshall and Olivia Wilkinson, What’s faith got to do with COVID-19? Apart from being well qualified to contribute, they cover an important topic. The role of faith is central, in terms of response and providing people succour and meaning.
By now we know that almost all recover from this virus, some are not even aware they are infected. Those who do end up in hospital, on oxygen or ventilators, are seriously ill and may suffer long term ill health. A small number die. Mortality from Covid-19 is higher than seasonal flu, although much below SARS, MERS and the bird flus of the last two decades. The distinguishing features are the period of asymptomatic infectiousness; the highly contagious nature of the virus; lack of treatment; the astronomical numbers we are seeing; the incredible disruption to lives, including the economic catastrophe we are facing; and the sense we do not yet have answers – either vaccines or treatment.
The Numbers
Table 1 shows the top nine countries (and China) by total number of cases. There has been little movement in ranking, but the numbers climb across the world. The Chinese epidemic is static, it is included as the source of the epidemic. It will be excluded from next week. Four of the top nine are Latin American countries. There is one Asian and one African nation in the Table: India and South Africa. The UK and Russia are the only two European nations with sufficient cases for inclusion.
| Date | Global cases | Brazil | Chile∞ | China | India∞ | Mexico∞ | Peru∞ | Russia | South Africa | UK | USA |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 15 Feb | 69,000 | 0 | 68,400 | 2 | 0 | 9 | 43 | ||||
| 4 Mar | 93,000 | 4 | 80,480 | 3 | 0 | 86 | 149 | ||||
| 18 Mar | 201,500 | 372 | 81,100 | 147 | 116 | 2,600 | 7,800 | ||||
| 1 Apr | 861,000 | 6,836 | 82,400 | 2,777 | 1,400 | 29,900 | 213,400 | ||||
| 15 Apr | 1,982,552 | 28,280 | 83,351 | 24,490 | 2,415 | 94,845 | 609,422 | ||||
| 29 Apr | 3,117,756 | 79,685 | 83,940 | 93,399 | 4,996 | 162,350 | 1,012,583 | ||||
| 13 May | 4,262,799 | 180,000* | 84,018 | 232,243 | 11,350 | 227,741 | 1,369,964 | ||||
| 27 May | 5,594,175 | 291,222 | 84,103 | 362,342 | 24,264 | 241,408β | 1,681,418 | ||||
| 10 Jun | 7,250,909 | 739,503 | 84,198 | 493,023 | 52,991 | 262,098 | 1,979,893 | ||||
| 24 Jun | 9,264,569 | 1,145,906 | 264,689 | 84,653 | 456,183 | 196,847 | 264,689 | 598,878 | 106,108 | 277,200 | 2,347,022 |
| 8 Jul | 11,830,885 | 1,668,539 | 312,911 | 84,917 | 742,417 | 261,750 | 312,911 | 693,215 | 215,885 | 286,979 | 2,996,098 |
| 15 Jul | 13,323,530 | 1,926,824 | 319,493 | 85,226 | 936,181 | 311,486 | 333,867 | 738,787 | 298,292 | 292,931 | 3,431,754 |
| 23 Jul | 14,959,031 | 2,159,135 | 334,683 | 85,314 | 1,193,078 | 356,255 | 362,087 | 787,864 | 381,798 | 297,389 | 3,902,135 |
* estimate ∞ these countries were added and so the early data has not been extracted. β Data for the UK from Worldometer
When I first produced a table, on 8th April, it was to try to make sense of the data. I had a column for South Korea since they briefly (for just one week) had the second largest number of cases in the world. At that point France, Italy and Spain also merited inclusion. It is difficult to make sense of the French data, on some days no cases are reported and then a thousand will be shown the next.
It is hard to compare absolute numbers when populations are so different. To make useful assessments we need to look at rates as is done in Table 2.
| China | France | Italy | Russia | South Korea | South Africa | Spain | UK | USA | |
|---|---|---|---|---|---|---|---|---|---|
| Deaths (19 May) | 3.33 | 421.07 | 529.64 | 18.84 | Error* | Error* | 593.04* | 523.33 | 275.8 |
| Total cases (20 May) | 58.4 | 2,189 | 3,736 | 1,991 | 216 | 277 | 4,953 | 3,629 | 4,557 |
| Deaths (26 May) | 3.33 | 424.27 | 544.04 | 25.15 | 5.21 | 8.32 | 574.31 | 555.19 | 299.79 |
| Total cases (25 or 26 May) | 58.4 | 2,225 | 3,806 | 2,421 | 216 | 398 | 5,034 | 3,847 | 4,964 |
| Deaths (3 June) | 3.33 | 429.83 | 533.93 | 33.56 | 5.27 | Error* | 580.58 | 587.24 | 320.93 |
| Total cases (2 or 3 June) | 58.4 | 2,320 | 3,856 | 2,905 | 225 | 579 | 5,125 | 4,070 | 5,472 |
| Deaths (17 June) | 3.33 | 438.73 | 568.76 | 49.01 | 5.38 | 27.14 | 580.78 | 627.71 | 354.46 |
| Total cases (16 or 17 June) | 58 | 2,410 | 3,924 | 3,681 | 237 | 1,239 | 5,221 | 4,372 | 6,386 |
| Deaths (23 June) | 3.33 | 442 | 573 | 59 | 5 | 38 | 606 | 865 | 370 |
| Total cases (22 or 23 June) | 58 | 2,462 | 3,942 | 4,058 | 243 | 1,712 | ° | 4,497 | 6,985 |
| Deaths (1 July) | 3.33 | 444 | 574 | 63 | 5 | 43 | 606 | 655 | 385 |
| Total cases (30 June or 1 July) | 58 | 2,516 | 3,976 | 4,393 | 249 | 2,432 | ° | 4,595 | 7,826 |
| Deaths (8 July) | 3 | 444 | 575 | 64 | 5 | 46 | 606 | 657 | 388 |
| Total cases (7 or 8 July) | 59 | 2,759 | 3,999 | 4,713 | 257 | 3,317 | ° | 4,209 | 8,877 |
| Deaths (15 July) | 3 | 447 | 578 | 80 | 5.6 | 75 | 608 | 676 | 416 |
| Total cases (14 or 15 July) | 59 | 2,640 | 4,024 | 5,070 | 264 | 5,029 | 5,488 | 4,292 | 10,367 |
| Deaths (22 July) | 3 | 450 | 580 | 85 | 5.7 | 89 | 608 | 681 | 430 |
| Total cases (21 July) | 59 | 2,707 | 4,045 | 5,327 | 269 | 6,299 | ° | 4,351 | 2,949 |
*misread these data °data missing
Terminology
Recovery
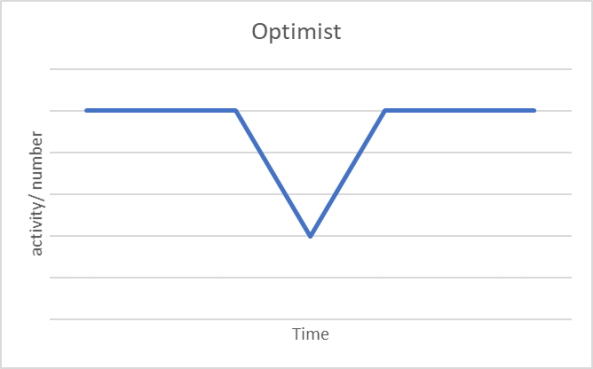
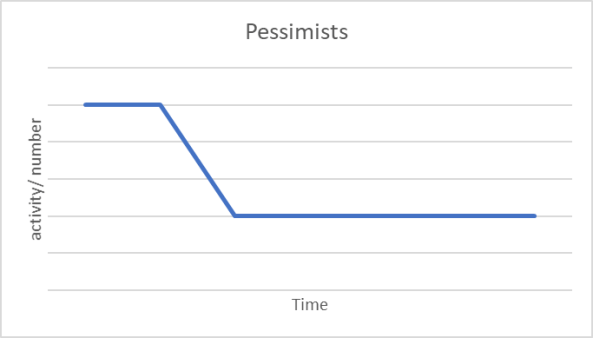
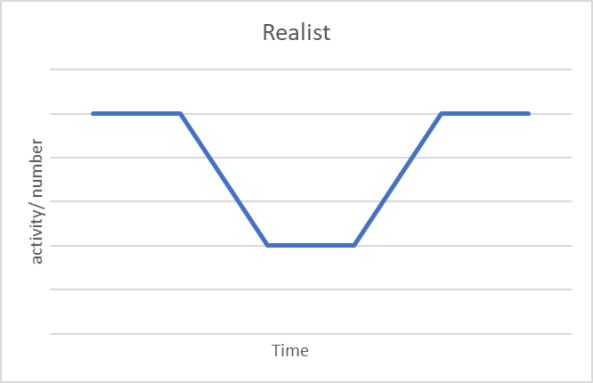
There are debates over the shape of the collapse and recovery. Optimists talk of a V: there is a steep decline in, say, economic activity, but it bounces back, hopefully to the levels before Covid-19. Pessimists suggest it will be an L: after the decline activity remains at low levels. The so-called Realists believe it will be U shaped: the steep decline, followed by low levels of activity and then, after an unspecified time, a recovery to close to pre-Covid levels.
In my view none of these reflect what will actually happen. We have seen the decline, so we know what one half of the graph looks like. We hope we are at the lowest point. This may not be the case, it depends on the success of interventions, feedback loops and consumers (both confidence and spending powers). I believe the curve will be a series of ‘waves and wobbles’ with gains and losses over a long period of time, probably as long as three years. These different graphs are on Figure 1. The curves are most often assumed to refer to economic indicators. The patterns they show could be applied to many indicators: travel, meals out, jobs and so on. Many of the macro-interventions are designed to restore confidence and economic activity. In my view they should rather be seen as temporary social transfers.
Figure 1: prospective epidemic curves; optimist, pessimist, realist, waves and wobbles

The epidemic will not end soon. There will be changes to the way we live, and most people will be losers. The airline industry illustrates this.
“As states started to reopen and passengers started flying again, airlines began to believe that the worst was behind them, and travel was on its way back. But then, things began to change as the virus started to surge in leisure destinations – places where travel demand was high. Florida, Texas, Georgia, Arizona, California, Nevada, South Carolina, and other popular summer destinations are all experiencing a surge in cases that has then led to a decline in bookings and, thus, revenue. This has led airlines to start to pare back capacity and re-evaluate growth.”4
I personally love travel and aircraft. It will be a long time before I happily take a long-haul flight, not because I fear being infected, but because the experience would not be pleasant. The thought of wearing a mask for a twelve-hour flight does not appeal. The environment is also a major concern.
In 1994 journalist and public intellectual Laurie Garrett published THE COMING PLAGUE: Newly Emerging Diseases in a World Out of Balance. The book warned of what could happen, especially given the belief then that humans could conquer disease. The virus causing the greatest concern then was AIDS, and it was published two years before an effective treatment became available.5 Despite the warnings in this book, and her subsequent writings, Covid-19 emerged into an unprepared and complacent world, as Richard Horton noted in his book (reviewed on 9th July).6 Garrett is a commentator worth following.
Super-spreading events and super spreaders
The term ‘super-spreading’ suggests one person can infect tens or hundreds of others. This has happened, the choir in Washington State and church service in South Korea were identified earlier in the year. I have given the Morbidity and Mortality Weekly Review reference for the choir. The title was ‘High SARS-CoV-2 Attack Rate Following Exposure at a Choir Practice’.7 The Los Angeles Times ran the South Korean story under the headline ‘A choir decided to go ahead with rehearsal. Now dozens of members have COVID-19 and two are dead’.8 The potential for blame and stigma is self-evident.
Due to the period of infectiousness before symptoms develop an individual can, potentially and inadvertently, infect many others. This means the track and trace public health response is crucial, and this requires rapid and reliable antigen tests. Super spreading events would include football matches, concerts, political rallies, and other large gatherings. Wearing face masks greatly reduces risk. This was well illustrated by the large global ‘Black Lives Matter’ protests and marches, which did not result in an increase of infections. I hope no one will be referred to as a ‘super spreader’.
Waves, peaks, and spikes
The discourse includes terms such as ‘second wave’, the ‘peaks of infection’ and ‘spikes in infection’. In my view this discourse is not helpful as it is inaccurate and misleading. I am not sure how to change it. To believe there will be a second wave as large as the first is to assume we have not learnt anything, this is clearly not true. Referring to a ‘peak’ early in the epidemic is to assume foresight that is problematic. Peak is singular, there can only be one and we need to be sure when we have reached and passed it.
One of the key needs is good data and observers. In the UK we were shocked to learn the death data were unreliable. According to the Guardian quoting Yoon K Loke and Carl Heneghan, of the Centre for Evidence-Based Medicine at Oxford University:
“It seems that PHE regularly looks for people on the NHS database who have ever tested positive, and simply checks to see if they are still alive or not. PHE does not appear to consider how long ago the Covid test result was, nor whether the person has been successfully treated in hospital and discharged to the community. A Department of Health and Social Care source summed this up as: “You could have been tested positive in February, have no symptoms, then be hit by a bus in July and you’d be recorded as a Covid death.”9
Guest spot: What’s faith got to do with COVID-19? by Katherine Marshall, Olivia Wilkinson10
In early March, three individuals, with the support of our organizations launched an effort to track how the world’s different religious communities and institutions were responding to the COVID-19 emergency. Katherine and Olivia (the two authors) and Dave Robinson had all followed the 2014-5 Ebola crisis intensively, seeking insights into what worked and what did not, and looking to lessons as to how religious dimensions could and should be more integrally part of the strategic framework for response. We had pursued similar reflections on other pandemics, especially HIV and AIDS, malaria, Tuberculosis, and Zika. Thus, with early reports making it clear religious bodies were deeply involved in COVID-19: we started to gather information in a resource repository; began to send out daily highlights; organized a webinar series to learn more about what was happening in different regions; and shared ideas in the form of blogs and articles. The tempo is shifting as the pandemic approaches the half year mark, and, while uncertainties lie ahead, useful insights have emerged.
What we know
More obviously and sooner than in earlier pandemics, the role of religious entities was noted in many quarters. The reasons were largely negative: the prominent role of a Korean Church and a Muslim missionary organization as “super spreaders” of the virus, for example. WHO began to focus early, through EPI-WIN, a department focusing on epidemics and information, on working with faith institutions to convey messages, and, with inputs from various organizations, issued guidelines for faith communities, as did CDC and other organizations. As lockdowns emerged as an important part of the COVID response, the issue of religious gatherings took on increasing importance, both for religious bodies and in terms of government/religion relationships. Different practices were at issue, most prominently handling of dead bodies and funerals and shifting gatherings away from in-person to online meetings. Religious responses to the growing crisis of hunger, stress, domestic violence, and discrimination were expected and generous responses to vulnerable groups were observed.
Much information is available, primarily news accounts and reports from religious bodies, and an emerging body of surveys (e.g the Pew Research Center) and academic commentary. Most information, however, is anecdotal and fragmentary. It clearly suggests most religious communities have responded positively to the crisis; following public health guidance and cooperating in crafting and disseminating information. A minority have gone against the guidance. The outliers are individuals and denominations that continue to gather in-person and create further super-spreader events, and convey false or distorted information. While most interfaith groups actively counter stigma and discrimination, some contribute to such behaviours. This majority/minority position regarding public health guidance is echoed around the world, but with notable context-specific differences based on a country’s religious and political dynamics.
What we don’t know
Data on religious adherence and behaviour is notoriously partial and often elusive, sometimes deliberately so (where religious identity is excluded from census questions, for example). And the numbers are huge (involving some 80 percent of the world’s population, in widely diverse communities and entities). Thus, the task of gathering comprehensive information about religious responses worldwide is next to impossible, and inadvisable. The word “countless” is invoked often to indicate the unending extent of the task, but more importantly the diversity of religious beliefs and practices means that large-scale data sets miss vital nuances happening at very local levels. Country and more local-level surveys can help provide more detailed pictures, and in-depth qualitative research will be needed in time. There are several research projects of which we are aware that have shifted focus to COVID response and faith, but they are the work of years, rather than months. It is simply too early in the response to have primary data. Some scattered data points (for example surveys about prayer trends during the pandemic) offer inklings of initial insights. There are unknowns also about the impact, spiritual, psychological, social, and financial, of the lockdowns and losses and grief. And looking to the future, we can only begin to surmise the long-term impact on, for example, faith-run education and health care and adherence to different communities. These aspects will provide researchers with questions for years to come. We hope that our repository of daily updates will provide some basis of information for such researchers.
What’s especially important
An impetus for the project was awareness of lessons we learned from previous pandemics. Three stand out: the vital importance of community mechanisms in responding to health crises; the benefits of well-established and meaningful consultative mechanisms involving governments and religious bodies; and the benefits of effective work on preparedness. As with previous epidemics, faith communities are found in every aspect of the response. Where they deliver large shares of health, education, and social protection, their roles are vitally important. Positive responses to domestic violence and to the obvious effects of stress and mental health amidst the crisis are something to watch and understand better as they emerge as areas of special interest.
While many religiously linked entities, including large NGOs and some academic organizations, took careful note of the lessons learned from previous pandemics about faith engagement, there are significant gaps. A key lesson is religious actors are often not at policy making tables and operate in parallel to official responses rather than in coordination; they should be at the table, given their reach, trust, and experience. Focusing in on our area of work, there are some indications that international organizations and governments recognize the role of faith actors more fully, marking the continuation and growth of an awareness of faith in international development and humanitarian work. Yet consultations remain superficial and occur only after the crisis had started.
What maybe is less so
Trying to separate out religious from non-religious community responses is not useful (though it is frustrating to see how often reviews of civil society responses simply exclude or ignore their religious dimensions). There is a blending in communities across the world, faith and non-faith, especially at the vital local level. That applies also to questions about what motivates people and where effective leadership comes into play. Key is to see religious identities, behaviour motivator, and institutions as integral parts of the broader context and environment, not isolated or essentialized factors.
Much is written about “faith versus science”. While some religious people and communities deliberately reject health and medical guidance, they are outliers and misdirect the debate towards one of opposition rather than an understanding that these are not mutually exclusive positions. The effort to see a tension and separation can be a red herring.
Historically, pandemics have marked turning points, followed often by significant social and religious transformations. It remains to be seen how the COVID-19 emergency will have similar transformational effects. Some studies have claimed the pandemic has prompted a “return to religion” in contexts where religious affiliation was fading – this is a claim seen after other crises, but with varying evidence of long-term effects. Again, it is too early to tell at a societal level and making predictions while the situation is still developing can lead to incorrect presumptions.
Areas to watch
Religious relationships with governments are challenged and tested during the COVID-19 crisis and bear watching: will new tensions emerge, is it possible better understandings can be built? Longer term impacts of lockdowns and trauma on communities will likewise have unanticipated effects. Constructive roles of religious actors in the hoped-for efforts to reimagine, redesign, and “build back better”, notably by addressing inequalities in a more forthright manner, are much needed, as are their peacebuilding skills in addressing ongoing conflicts and new ones that are emerging.
Conclusion
This epidemic is not homogenous, and it is complicated. The ‘big new idea’ this week is to put into simple graphs the epidemic curves we might see. It would be good to put values on the x and y axis, recognising they would vary by country and region. Not covered are the differential consequences. As I completed this blog, I was made aware of work from the UNICEF Research office on children. This will be covered next week.
The question of how to respond in different settings is also a concern and Canadian academic Stephen Hodgins has discussed if Higher-Income Country responses are appropriate in Low and Lower-Middle-Income Countries. The paper is included in the references. We must also be aware of the greatly increased mental health issues. The Kaiser Family Foundation found these have increased; average weekly data for June 2020 found that 36.5% of adults in the U.S. reported symptoms of anxiety or depressive disorder, up from 11.0% in 2019.11
References
Lynne M. Mofenson et al, The Evolving Epidemiologic and Clinical Picture of SARS-CoV-2 and COVID-19 Disease in Children and Young People, UNICEF Office of Research, Innocenti Working Paper WP-2020-07 July 2020
Heather Farmbrough, Why Sweden’s Approach To Coronavirus May Not Be What You Think, Forbes http://www.forbes.com/sites/heatherfarmbrough/2020/05/14/why-swedens-approach-to-coronavirus-may-not-be-what-you–think/#19dc05622464
Stephen Hodgins, Abdulmumin Saad, Will the Higher-Income Country Blueprint for COVID-19 Work in Low- and Lower Middle-Income Countries?, Global Health Science and Practice https://www.ghspjournal.org/content/early/2020/06/13/GHSP-D-20-00217
Thank you for reading, reposting and providing comments. What I write is public domain so please share, forward and disseminate. My contact is: awhiteside@balsillieschool.ca
- These data are from Johns Hopkins University https://coronavirus.jhu.edu/map.html
- The UK data from 27th May is taken from Worldometers.info.coronavirus/country/uk
- Deaths http://www.statista.com/statistics/1104709/coronavirus-deaths-worldwide-per-million-inhabitants/
Case per million ourworldindata.org/grapher/total-confirmed-cases-of-covid-19-per-million-people - Jay Singh, ‘US Passenger Growth Begins To Stall As Virus Surges. Simple Flying’, July 20, 2020 https://simpleflying.com/us-passenger-numbers-stall/
- Laurie Garrett, ‘THE COMING PLAGUE: Newly Emerging Diseases in a World Out of Balance’, Farrar, Straus and Giroux, 1994
- Richard Horton, The COVID-19 Catastrophe: What’s Gone Wrong and How to Stop it Happening Again, Polity Press, Cambridge, 2020
- Lea Hamner, et al, High SARS-CoV-2 Attack Rate Following Exposure at a Choir Practice — Skagit County, Washington, March 2020 Morbidity and Mortality Weekly Review, May 15, 2020 / 69(19);606–610 https://www.cdc.gov/mmwr/volumes/69/wr/mm6919e6.htm
- Raphael Rashid, Being Called a Cult Is One Thing, Being Blamed for an Epidemic Is Quite Another, How one mysterious church became a lightning rod for South Koreans’ anger over the coronavirus outbreak. New York Times March 9, 2020
- https://www.theguardian.com/world/2020/jul/21/analysis-why-englands-covid-19-death-toll-is-wrong-but-not-by-much
- Katherine Marshall is Senior Fellow at Georgetown University’s Berkley Center for Religion, Peace, and World Affairs and Executive Director of the World Faiths Development Dialogue (WFDD). km398@georgetown.edu
Olivia Wilkinson, PhD, is Director of Research at the Joint Learning Initiative on Faith and Local Communities. - https://www.kff.org/statedata/mental-health-and-substance-use-state-fact-sheets/
Excellent resources this week, Alan! Thanks especially for the https://www.lauriegarrett.com/ link. Hope you’re very well.
Asia Nelson, Founder – Movement Flow & Yoga Teacher Training Pranalife Yoga – pranalifeyoga.com The Movement Life – themovementlife.com Get the EMAIL
LikeLike